A 5-year-old FS Pit Bull Terrier dog presented for not acting right per owner, vomiting for one day, and anorexia. Temperature was normal. Initial blood chemistry revealed azotemia, low cholesterol, hyperamylasemia, and low triglycerides. CBC found thrombocytopenia. Total T4 and Pancreatic Lipase Immunoreactivity were both normal. Within a few weeks, the patient was examined again due to a decreased appetite, decreased drinking, diarrhea, several episodes of vomiting, and the possibility of toxin exposure. The dog was then admitted to the hospital for I.V.
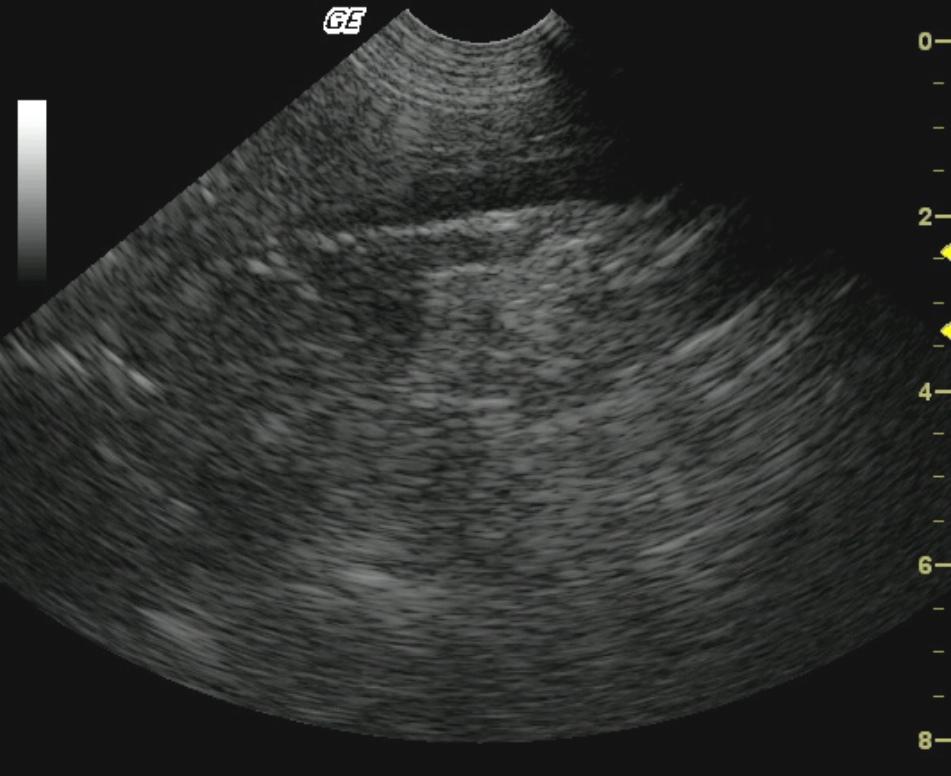
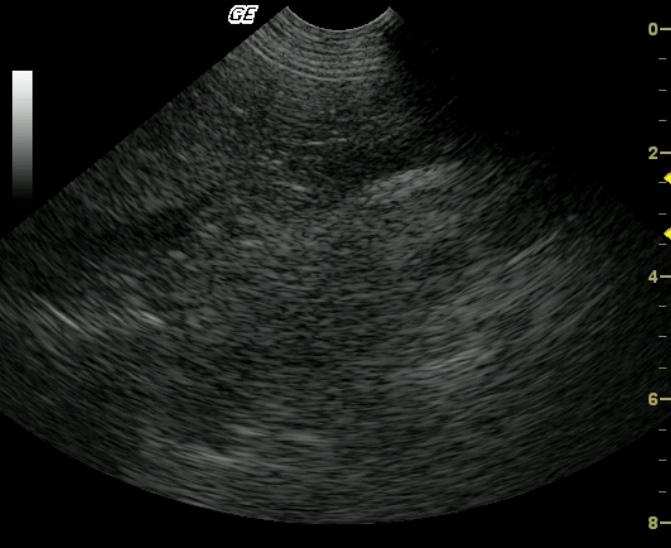
A 5-year-old FS Pit Bull Terrier dog presented for not acting right per owner, vomiting for one day, and anorexia. Temperature was normal. Initial blood chemistry revealed azotemia, low cholesterol, hyperamylasemia, and low triglycerides. CBC found thrombocytopenia. Total T4 and Pancreatic Lipase Immunoreactivity were both normal. Within a few weeks, the patient was examined again due to a decreased appetite, decreased drinking, diarrhea, several episodes of vomiting, and the possibility of toxin exposure. The dog was then admitted to the hospital for I.V. fluid therapy, blood work, urinalysis, ACTH stim., and abdominal ultrasound. Physical exam found patient weak with a doughy abdomen, depressed mentation, slight tachycardia with thready pulses, tacky mucous membranes, and five pounds of weight loss in 1.5 months. Recheck blood chemistry revealed hypoglycemia, azotemia, hyperkalemia, and hyperamylasemia. CBC was within normal limits. Urinalysis showed a normal pH and specific gravity. Hypoadrenocorticism was diagnosed on the ACTH stimulation test.
Hypoadrenocorticism. Gastroenteritis – dietary indiscretion, infectious such as bacterial, viral, or fungal), foreign body ingestion with secondary obstruction and perforation causing the dog to go into shock, intestinal accident such as an intussusception or volvulus, severe case of inflammatory bowel disease with possible secondary lymphangiectasia, ascites and shock. Thrombocytopenia – DIC, lymphoma (paraneoplastic syndrome), leptospira sp. infection, immune-mediated thrombocytopenia with hemorrhaging into the brain, lab error. Azotemia – neoplasia (lymphoma, adenocarcinoma, leiomyoma, leiomyosarcoma, mast cell tumour) with secondary azotemia and a possible perforation of the intestine (+/- DIC as cause of the thrombocytopenia), toxin ingestion (xylitol, raisins, ethylene glycol) causing secondary renal failure and shock, renal failure (acute on chronic) secondary to leptospira sp. infection, chronic renal insufficiency.
Patient was put on regimen of Percorten injections and steroids with the advisement of rechecking blood work in 12 days. Electrolyte profile showed only hypernatremia. Azotemia and hyperamylasemia were still present. Recheck urinalysis a few months later showed high Ph and low specific gravity. Urine culture was negative. Blood pressure was elevated at 170. Urinalysis two months later showed a normal Ph, low specific gravity, a cloudy appearance, trace proteinuria, hematuria, elevated RBC, and the presence of Calcium oxalate crystals. Patient presented again (9/1/05) for vomiting and polydipsia, and was admitted to hospital for I.V. fluid therapy, urinalysis, urine culture, and abdominal ultrasound. Blood chemistry revealed hypoglycemia, low BUN, hypoalbuminemia, high ALT, high AST, hypernatremia, low A/G ratio, hyperglobulinemia, and hyperamylasemia. CBC, T-4, and Bile Acids profile were all within normal limits. Urinalysis showed high Ph, low specific gravity, and hematuria. ACTH stim. still found hypoadrenocorticism. Annual exam (3/13/06) found patient doing well. Azotemia had resolved, although chemistry still found the presence of hypoalbuminemia, low A/G ratio, hyperglobulinemia, and hyperamylasemia. CBC revealed thrombocytopenia. T-4 was normal. ACTH stim. again found hypoadrenocorticism. TLI, B12, and Bile Acid Profile were all within normal limits. Folate was low. Patient was once more admitted to the hospital (3/23/06) for I.V. fluid therapy and close monitoring of PCV/TP due to thrombocytopenia. Follow-up blood chemistry, CBC, and T-4 (7/06/06) were all normal.