– 7 year old MN Sheltie acute onset vomiting and diarrhea
– bloodwork showed mild elevation ALT, elevated ALP, GGT and bilirubin
– positive SNAP cPLI
– scan performed after 48hrs IV fluids, cerenia, famotidine, sulcrate, antibiotics and ursodiol
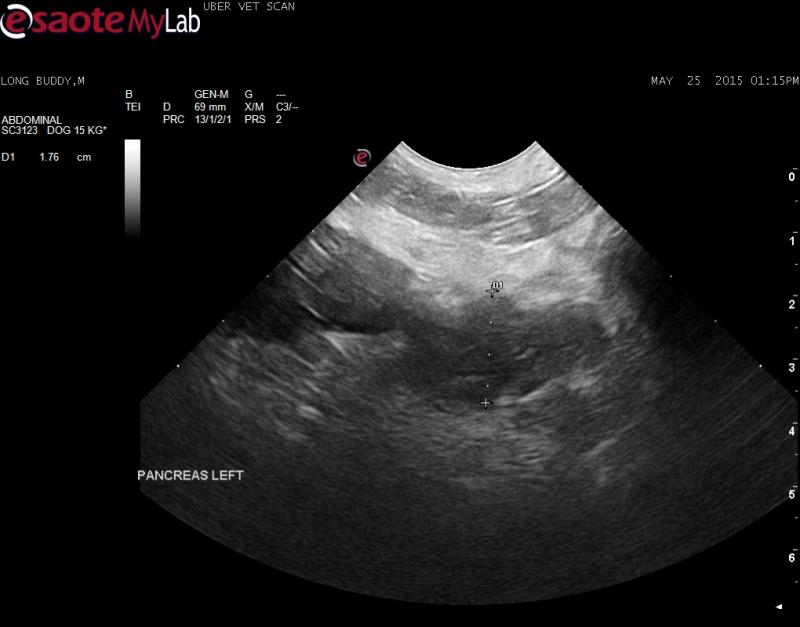
– hypoechoic right and left limb of the pancreas with hyperechoic surrounding fat; pain over the right limb
– 7 year old MN Sheltie acute onset vomiting and diarrhea
– bloodwork showed mild elevation ALT, elevated ALP, GGT and bilirubin
– positive SNAP cPLI
– scan performed after 48hrs IV fluids, cerenia, famotidine, sulcrate, antibiotics and ursodiol
– hypoechoic right and left limb of the pancreas with hyperechoic surrounding fat; pain over the right limb
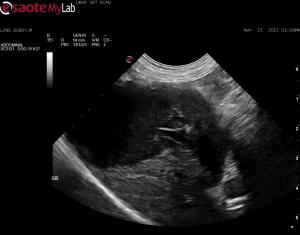
– GB distended with granular looking bile, linear hyperechoic echos and some adherent hyperechoic sludge to the walls; liver is hypoechoic to falciform fat; there is alot on inflammation around teh stomach
– the cystic duct is distended but I could not find evidence of distension of the biliary tree elsewhere; no surrounding inflammtion and no pain over the GB
– Repeat bloodwork showed improved ALT but now worsening of ALP, GGT and bilrubin
What is your opinion of this gall bladder and liver? Emerging mucocele? Cholangiohepatitis? Could the increase in liver enzymes just be response to the pancreatitis?
This is a money case so GB surgery is out of the question – I would prefer to give the patient just pancreatitis 🙂 I have offered to rescan for free if I get called into this clinic again with another case pending clinical outcome

8 responses to “Pancreatitis and distended GB”
There is striating bile,
There is striating bile, oversdistended Gb and cystic duct, and increased portal markings in the liver… panc and mucoceles go toether especially in a sheltie… the king of mucoceles:) Lots of reactuve mesentery and gastric thickening too. Need to zoom in on th ecbd in these cases and wade through the echo artifact to see what is going on there. I would tx panc first and watch the WBC, SAP, bili, and alt and progress… may need the gb out but remember with right panc you can always a certain level of stasis from post hepatic obstruction and the Gb will distend from anorexia. I think emerging mucocele applies here but may need removal in days or months. Once eating again could do a Gb motility study.
There is striating bile,
There is striating bile, oversdistended Gb and cystic duct, and increased portal markings in the liver… panc and mucoceles go toether especially in a sheltie… the king of mucoceles:) Lots of reactuve mesentery and gastric thickening too. Need to zoom in on th ecbd in these cases and wade through the echo artifact to see what is going on there. I would tx panc first and watch the WBC, SAP, bili, and alt and progress… may need the gb out but remember with right panc you can always a certain level of stasis from post hepatic obstruction and the Gb will distend from anorexia. I think emerging mucocele applies here but may need removal in days or months. Once eating again could do a Gb motility study.
Thank-you EL!
Thank-you EL!
Thank-you EL!
Thank-you EL!
To EL,
Would you consider a
To EL,
Would you consider a one time anti-inflammatory dose of glucocorticoids for this case to help with potential pancreatic obstruction of the common bile duct?
To EL,
Would you consider a
To EL,
Would you consider a one time anti-inflammatory dose of glucocorticoids for this case to help with potential pancreatic obstruction of the common bile duct?
Hmm debatable because that
Hmm debatable because that stomach could be ulcerative… I would fna the hypoechoic portion of the right panc in video 1 and fna the liver and if predominant LP inflammation is the issue then yes more justified. But if after 48 hours of tx and the Gb is like that it needs to come out especially if bili is up. A dexemeth shot 0.25 mg/kg is a temp solution and could lead to perf…ive seen steroid anger up Gb mucoceles in multiple occasions… I would stabilize and go to sx if the gb hasnt emptied and bili is still up.
Hmm debatable because that
Hmm debatable because that stomach could be ulcerative… I would fna the hypoechoic portion of the right panc in video 1 and fna the liver and if predominant LP inflammation is the issue then yes more justified. But if after 48 hours of tx and the Gb is like that it needs to come out especially if bili is up. A dexemeth shot 0.25 mg/kg is a temp solution and could lead to perf…ive seen steroid anger up Gb mucoceles in multiple occasions… I would stabilize and go to sx if the gb hasnt emptied and bili is still up.